Overturn denials at scale with AI appeals

Denials rates are rising.
Manual appeals can't keep up.
84% of large insurers now use AI to process denials, turning decisions that once took days into seconds. Yet most health system teams are still appealing one at a time, spending hours each week on manual processes – with little insight into what's working.
The result? Denials go unchallenged. Patients face treatment delays. And 46% abandon treatment entirely – not because the care wasn't needed, but because the process to get it approved was.
Insurers have automated denials at scale. Now it's your turn. It's time to give your team the tools to fight back, and get your patients the care they deserve.
Your denial defense system
One platform. Streamlined integration. Smarter with every outcome.
Automate and scale denial management with Claimable.
<10
DAYS
AVERAGE RESPONSE
Unclog your RCM and get
patients answers, fast
OVER
80%
WIN RATE
More patients get approved for
needed care
15+
HOURS
SAVED PER APPEAL
Reduce the time and
staff it takes to appeal
$30+
MILLION
UNLOCKED VALUE
Proven success driving
care access in complex specialties
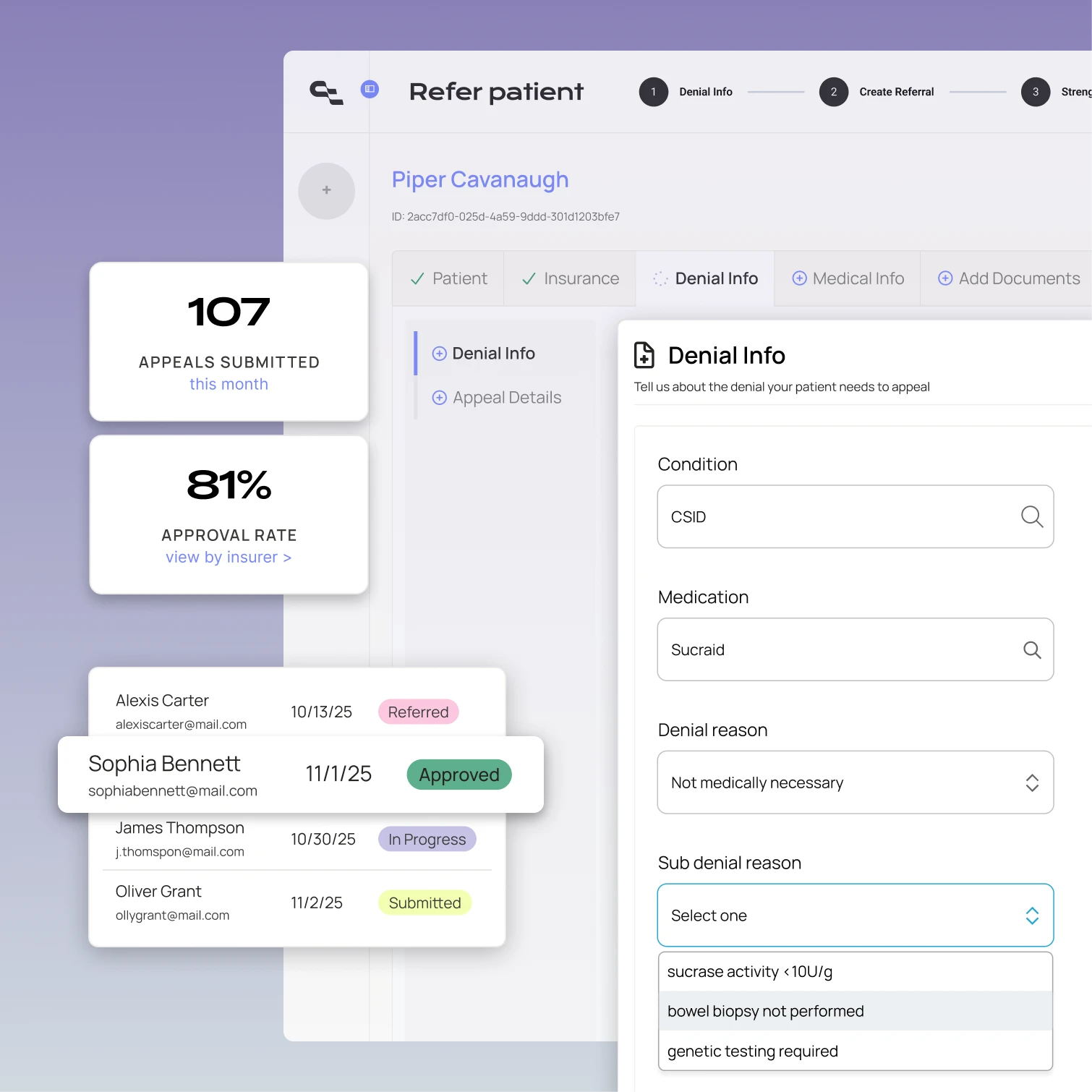
An integrated appeals solution
Claimable turns denial management from a cost center into an operational advantage – with seamless integration, enterprise-grade compliance and the sophistication to handle complex denials.
Connect to your existing EHR and RCM systems – no new platforms, no disruption to your workflow.
Generate physician-quality appeals in minutes, fully customized to every patient and denial.
Follow every appeal from submission to resolution – patients and staff always know where things stand.
Learn from every outcome to strengthen strategies, reduce denials, and improve operations.
Purpose-built for complex denials
Go beyond billing corrections and coding mistakes with an AI designed to handle complex care appeals.
From medical necessity to step therapy, Claimable's AI builds each appeal from clinical evidence, policy analysis, and legal leverage. Our proprietary database powers appeals with millions of evidence-strategy combinations tailored to each case – not templates insurers can learn to ignore.
✓ Trained on 4m+ clinical, legal and policy datapoints
✓ Customized to every denial, condition, insurer, and patient
✓ Continuously learning to make each appeal stronger


Stronger appeals, happier patients
Enhance your appeals workflow with the power of patient appeals.
Unlock additional levels of review and rights that only the patient can assert, giving you more ways to overturn every denial. Patients who go through Claimable feel supported, not sidelined. That shows up in outcomes, satisfaction scores, and your institution's reputation.
✓ Activate legal protections provider appeals can't access
✓ Seamless data flow for no extra burden on clinical staff
✓ Rated 5 stars on Google – patients love Claimable
See everything, improve everything
The denial intelligence your team has never had.
Claimable centralizes denial data into a real-time dashboard: which payers deny most, which therapies face the highest barriers, which strategies win. Powerful insights enable your teams to prioritize resources where patients are most at risk of losing access, and gives your contracting team real leverage at the negotiating table.
✓ Analyze by payer, therapy, denial type, and outcome
✓ Case-level tracking, so your team always knows status
✓ Denial pattern data arms payer negotiations and reduces future denials
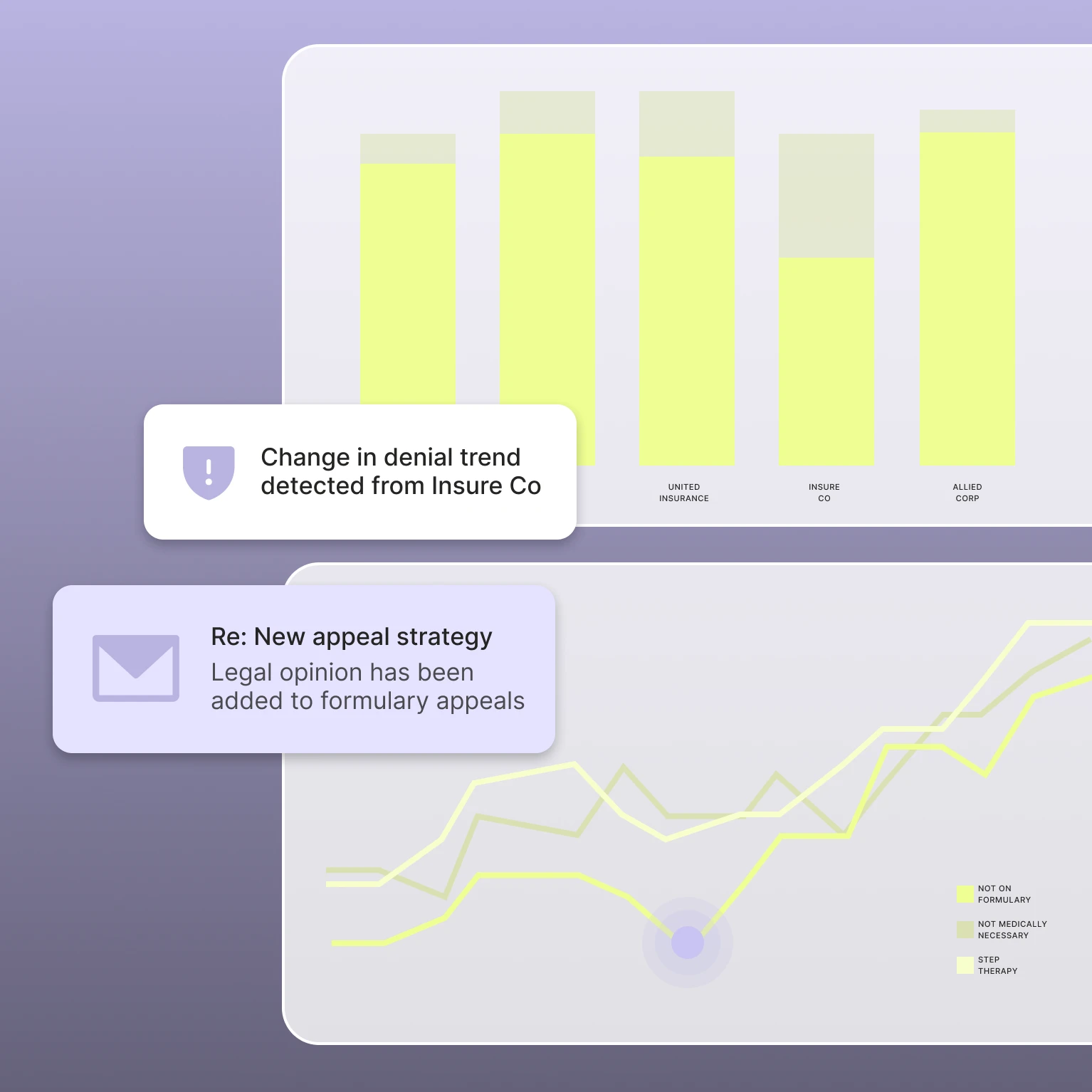

Seamless integration with your systems
Claimable's API-driven architecture integrates seamlessly with your existing tech stack. No new platforms to learn. No rip-and-replace.
Get your data flowing automatically – and give your staff an easy, centralized appeals dashboard that works alongside the tools they already use.
✓ API-driven architecture designed for existing EHR and RCM environments
✓ Multiple integration options from plug-and-play to bespoke
✓ Support materials and custom trainings for easy use
Automation built on compliance
Scale confidently with workflows designed for healthcare regulatory requirements from day one.
Designed for complex denials
Claimable's AI builds robust, clinically-backed appeals that justify coverage in complex situations, including those with limited clinical data and murky coverage criteria.

Oncology
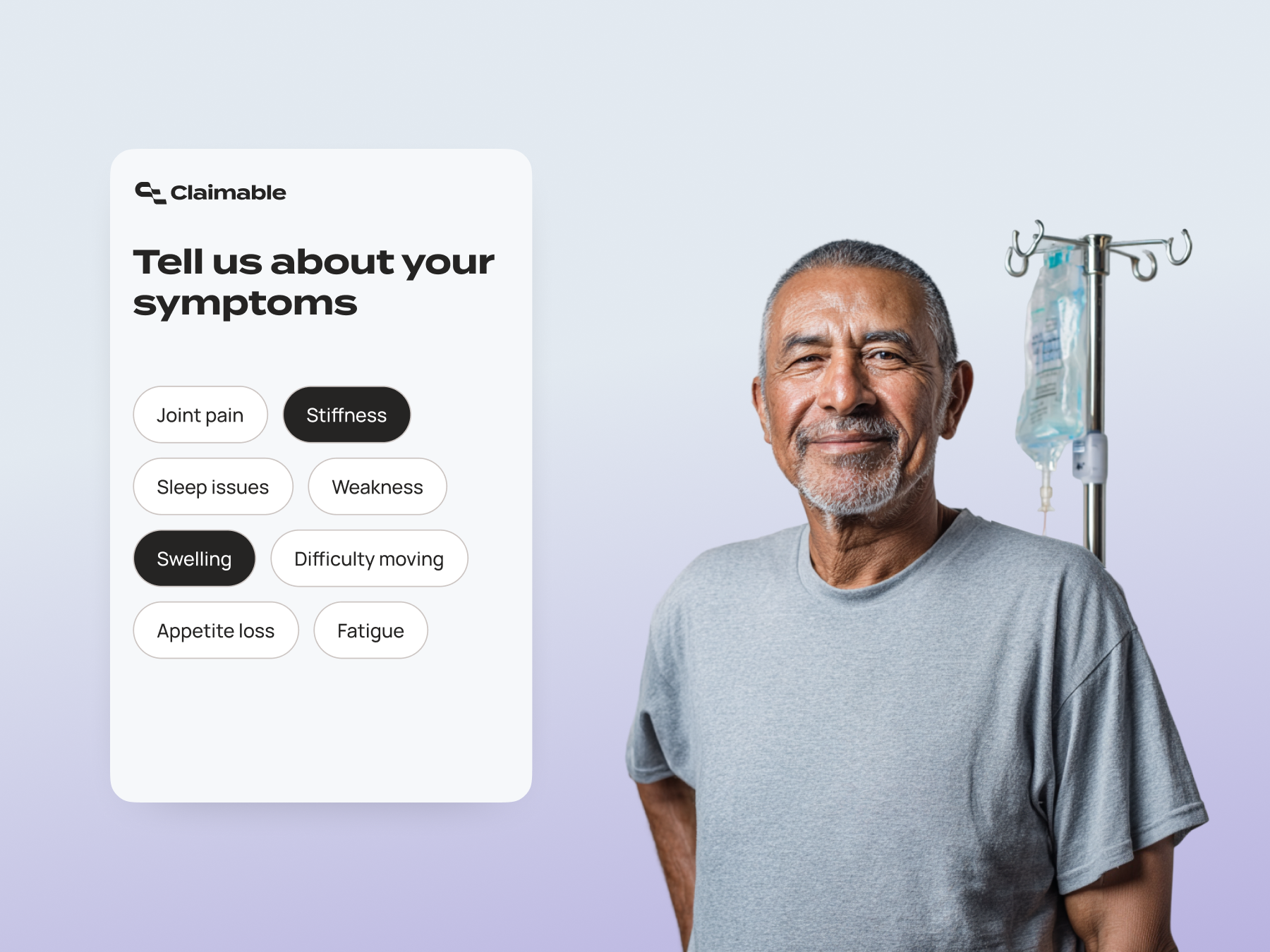
Infusion Centers
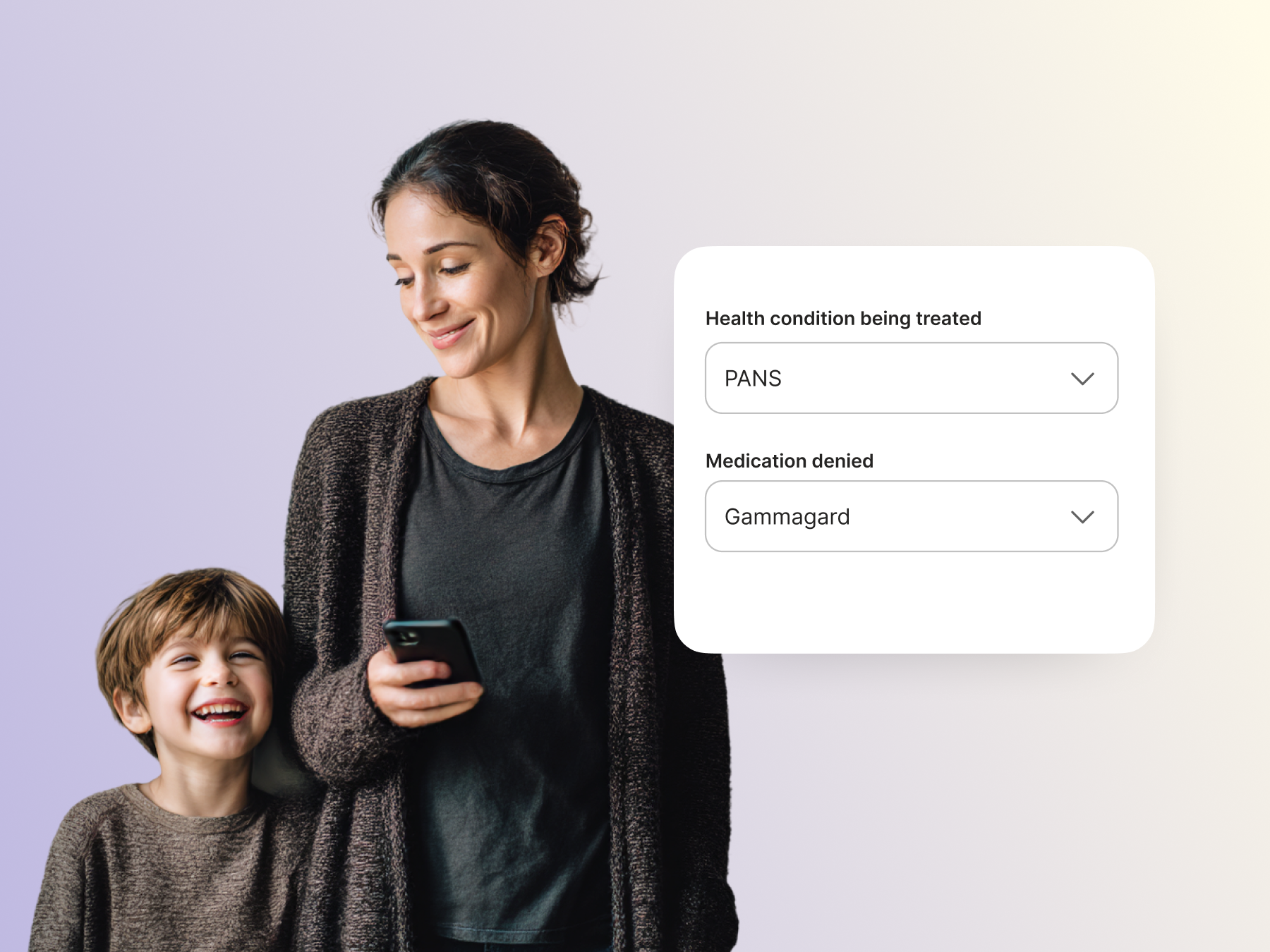
Rare Disease

Getting started is easy
1
2
3
Don't let denials decide who gets care.
See the difference Claimable can make: Drive efficiency, reduce RCM clog and improve patient satisfaction – all without adding admin work.










